
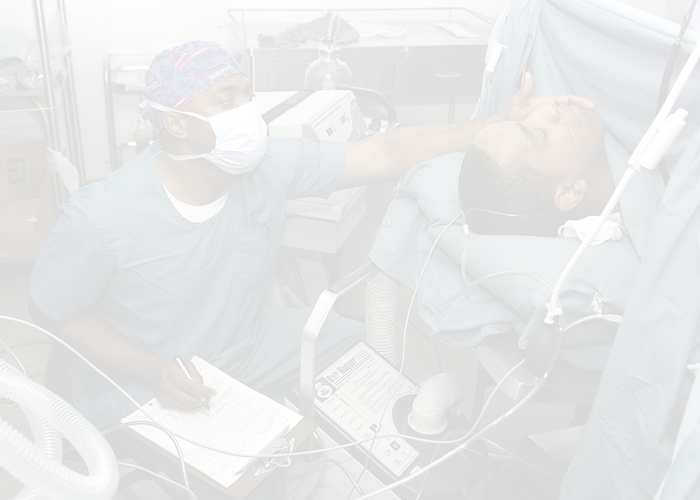
I put people into a coma, and the medications I administer cause paralysis. Yet only a handful of times each year do patients or family members ask how anesthesia actually works. The truth is there is much about anesthesia that even modern science can’t yet explain.
But I know, as sure as the sun rises in the morning, that when I add a gas to the inhaled breaths, loss of consciousness follows; and when I remove the gas, awareness returns. This is a harrowing responsibility, and one I never take for granted.
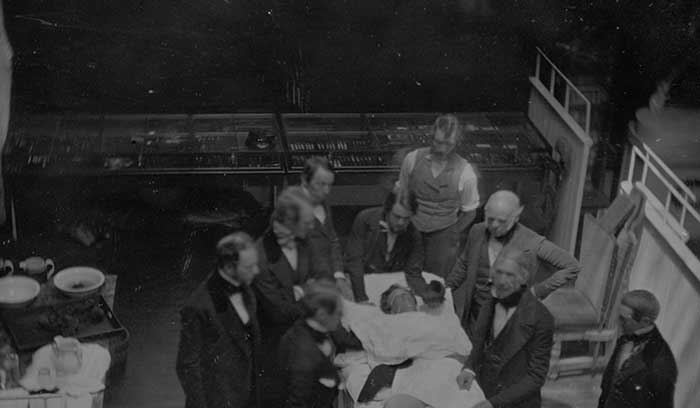
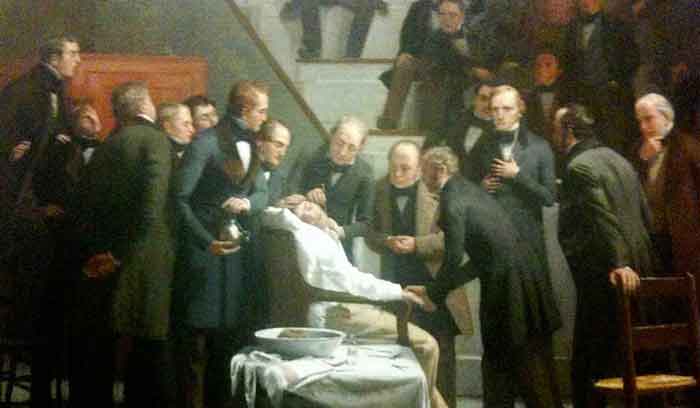
The renowned New England Journal of Medicine recently polled its readers to select the most important article the magazine had published in its distinguished history. The “resounding favorite” its readers settled on was the NEJM’s 1846 article by Henry Jacob Bigelow about the demonstration. This article, published just a few months after the historic demonstration at Mass General’s Ether Dome in Boston, bested every advance made since then, including the introduction of antisepsis, of X-ray imaging, and of antibiotics.
What does an anesthesiologist do?
The procedure for general anesthesia during a procedure entails a generic recipe: the big syringe (20 mL of a medication that causes a loss of consciousness), the little syringe (5mL of a paralyzing medication), and two clicks to the right (on the vaporizer that adds a gaseous anesthetic). Behind the simplicity of the recipe is a complex mix of aims, drugs, and techniques that extends anesthesia care beyond the actual anesthesia procedure, including pre-anesthesia patient preparation and post-procedure pain relief.
Since the discovery of ether, many adjunct medications have been added to the anesthesia gas to accomplish all-inclusive care. The effects that these side medications produce are what I call the “Five A’s of Anesthesia”:
- Anxiolysis, relieving stress created by an upcoming surgical procedure
- Amnesia, preventing memory formation during anesthesia care
- Analgesia, relieving pain during the procedure, but also considered beyond the procedure room to include post-procedure pain relief, acute (trauma) pain relief, and chronic pain relief
- Akinesia, preventing a patient’s movement during a procedure
- Areflexia, stopping adrenaline surge and swings in blood pressure and heart rate while under anesthesia
What is the difference between general and regional anesthesia?
Dating back to the Incas and through the nineteenth century, cocaine was used topically and injected into the spine to provide prolonged loss of sensation to the lower body without mental sedation—and thus regional anesthesia was born.
The use of regional anesthesia is expanding, with better and easier imaging techniques making it possible to accurately place current drugs on more nerves.
How does anesthesia provide relief from pain?
Regional anesthesia enters these nodes, blocking the signal jumps and thus the transmission of the pain signal beyond that point. General anesthesia induces a a complete insensibility to pain and all sensation. How exactly the inhaled gases work still remains a medical mystery.
What factors affect a patient's ability to receive anesthesia?
Age and weight are two crucial factors in determining which and how much of the complex mix of drugs and techniques that are used to put someone “under.”
Not all patients are able to tolerate anesthesia gas, and sometimes additional medications must be used. In such cases, amnesia must be a specific goal of the anesthesiologist, with medications for that purpose provided, or redosed if the procedure might outlast the actions of the amnestic drug.
Why can't I eat too close to receiving anesthesia?
The separate paths leading to the stomach and the lungs work on the either/or principle. Only one path may be open at a time, and eating and breathing are kept separate through a series of coordinated actions including muscles and reflexes. The vocal cords at the entrance to the trachea snap shut when food or drink enters the mouth. This reflex, the laryngeal adductor reflex, is beyond our active control and prevents any- thing in the mouth from going down the wrong pipe. To swallow, sphincters made of muscle in the esophagus relax and the contents of the mouth slide down into the stomach.
Acid is the anesthesiologist’s enemy. The stomach is capable of withstanding the acid it produces as an aid in digestion. But other tissue is not immune to this acid. Herein lies the risk of anesthesia, which relaxes muscles and turns off reflexes. The cinched esophageal sphincters relax, allowing the contents of the stomach to flow to the mouth while the laryngeal adductor reflex no longer guards the entrance to the trachea. To prevent aspiration under anesthesia, the stomach must be empty.





